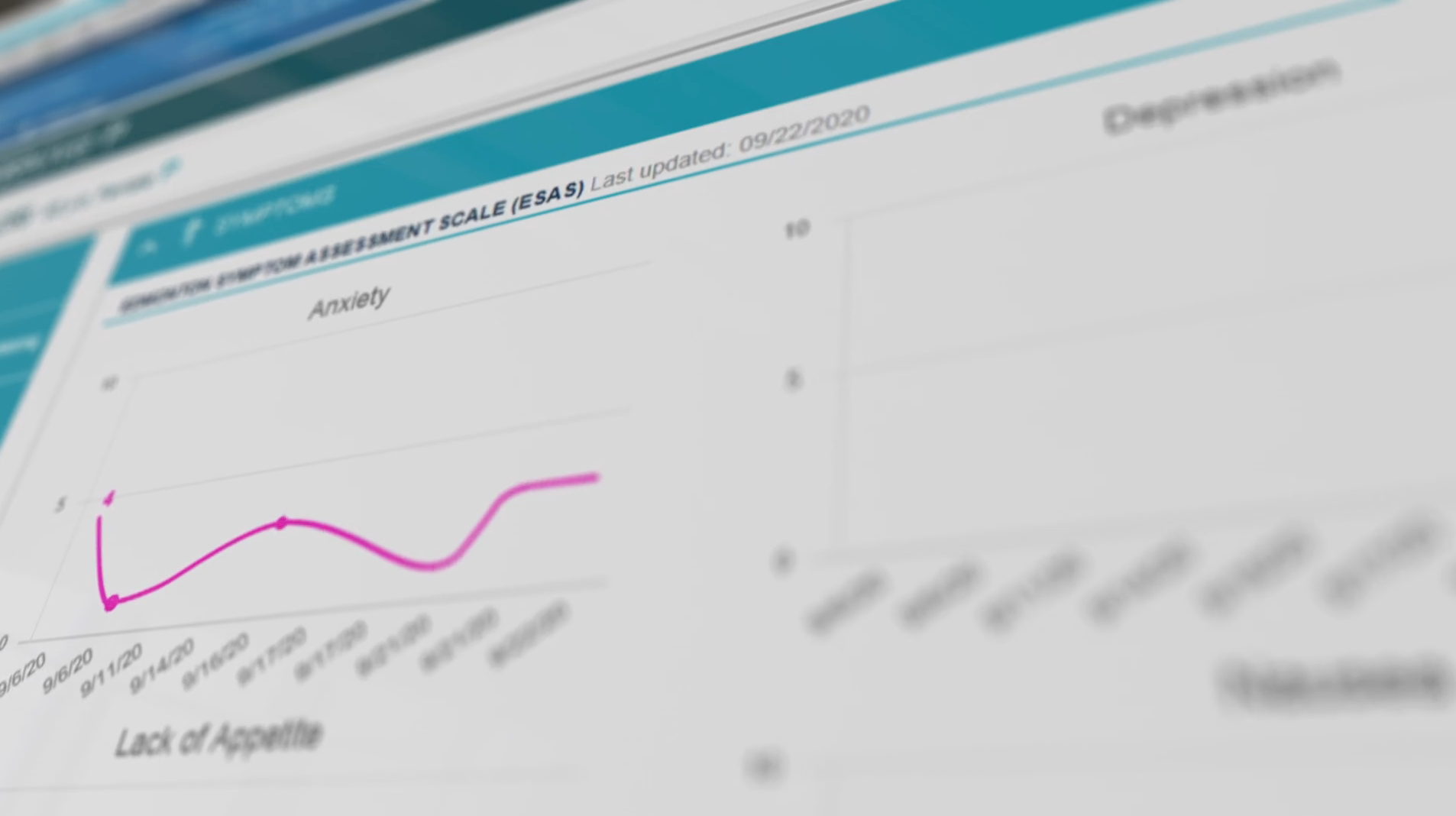
From the moment of cancer diagnosis, patients and their caregivers should have direct lines of communication to clinical care teams whenever they need them. When a patient experiences a physical symptom such as neuropathy (numbness and tingling of the hands and feet), he or she should be able to reach out to the team for immediate guidance on how to relieve that symptom.
While this is the ideal scenario, in practice it is difficult to achieve.
Although care teams strive to address patient symptoms as they occur, even when services are available, patients often do not feel comfortable reaching out to clinicians about their new or worsening symptoms. Most patients are keenly aware of how busy their oncology care teams are. Rather than “bothering” the team by reporting symptoms or asking questions about side-effect management between visits, patients often opt to wait until their next scheduled appointment. After delays of up to several weeks, it is quite common for patients to have “forgotten” the horrible symptom(s) they experienced right after treatment. Perhaps, in retrospect, the severity of the symptom does not seem so bad.
Sometimes, however, delays in reporting mild or moderate symptoms lead to more severe symptoms that require emergency department visits, hospitalizations, and potentially devastating delays in cancer treatment.
Cancer center protocols for patient communication with care teams vary. At one cancer center, patients may have 24/7 access to a triage nurse via a designated symptom call line. Another cancer center may tell patients to call the general number—often requiring the patient to wait on hold or leave a message for a nurse to call back. For patients experiencing a symptom(s), waiting on hold, or waiting for a call back can exacerbate their discomfort and discourage them from reaching out and receiving timely intervention.
Transitioning to Proactive Symptom Management
Moving from a reactive approach to a proactive approach for cancer symptom management is a goal for many cancer centers and care teams. Actions supporting a proactive approach includes patient outreach on a regular basis, and immediate feedback to patients based on patient reply. Operationalizing of this may include sending out regular symptom surveys and providing self-management strategies for mild symptoms reported. For those symptoms which require intervention, automated alerting to care team within the EMR is ideal for care teams to respond at the right time when patients are in need.
In this proactive approach, the lens through which care teams view symptom calls must change. Instead of being viewed as extra work or unplanned work, responding to patient calls and providing timely symptom management should be seen as a staple of caring for the patient when the patient needs the team most. Transitioning to a proactive symptom management approach enables timely interventions and higher quality, more-focused clinical decisions that ultimately result in better patient outcomes.
To read Reesa’s previous Nursing Perspectives blog post, click here.


