Using Technology to Improve Quality Metric Adherence
Paul Jacobsen, PhD1; Michele Gaguski, MSN, RN, AOCN, CHPN, APN2; Kathryn A. Thomas, BSN, RN, OCN, CCRP2; Amanda Hathaway, MD3; Karina I Halilova, MD, MPH3; Carrie T Stricker, PhD, NP4; Karen Hammelef, DNP, RN4; Sarahlena L Panzer, BS4; Douglas W. Blayney, MD5; Gabrielle Rocque, MD3
1MoffittCancerCenter (Tampa,FL); 2Atlanticare Cancer Care Institute(EggHarborTownship,NJ); 3University of Alabama Birmingham (Birmingham, AL);4Carevive Systems, Inc. (Miami, FL); 5Stanford University School of Medicine (Stanford, CA)
Background
- Many barriers to adherence to quality standards exist, including patient, provider, and system barriers to delivery and documentation of timely, evidence-based care
- Gaps s in clinician knowledge about care standards likely contribute to non-adherence
Method
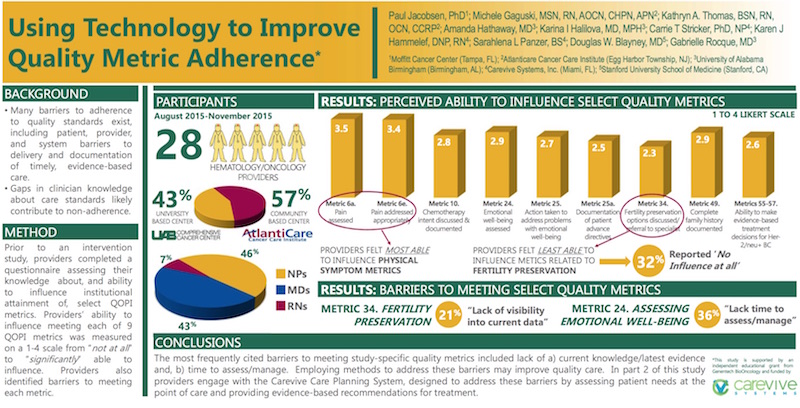
Prior to an intervention study, providers completed a questionnaire assessing their knowledge about, and ability to influence institutional attainment of, select QOPI metrics. Providers’ ability to influence meeting each of 9 QOPI metrics was measured on a 1-4 scale from “not at all” to “significantly” able to influence. Providers also identified barriers to meeting each metric.
Conclusions
The most frequently cited barriers to meeting study-specific quality metrics included lack of a) current knowledge/latest evidence and, b) time to assess/manage. Employing methods to address these barriers may improve quality care. In part 2 of this study providers engage with the Carevive Care Planning System, designed to address these barriers by assessing patient needs at the point of care and providing evidence-based recommendations for treatment.




